Story
Why Jerry Uses Humor with His OCD Patients
"It feels amazing to see someone who’s really struggling become the person they used to be. "
Clinical Expert: Jerry Bubrick, PhD
en EspañolEveryone says “you’re so funny.” Are you funny?
Jerry: I like to think I am. Using humor kind of softens a lot of what we do. If I can get a kid to laugh and see how ridiculous his thoughts and obsessions are, he’ll be that much more engaged in treatment.
When did you feel that this might be something you want to do as a career?
Jerry: When I was about nine years old, growing up in Minnesota, I was hanging out in my back yard with some friends in the middle of winter. Everything was white, covered in snow, and a dog, a black lab, was running towards us. Something in my brain just clicked and I had this panicked thought that the dog was going to attack us. So I got up instinctively and ran towards the house, and now the dog was chasing me and he thought we were playing. I made it into my house and closed the door and I saw him jumping and barking and having a great time, but I was terrified. For a year after that I was terrified of dogs. I wouldn’t go to someone’s house if there was a dog; I would cross the street to avoid them.
And then my parents instinctively did something that made me not afraid anymore. We got a dog. I remember watching my sisters play with him. He was licking them and they were having a great time. And I got more and more brave, and I reached over and started petting him, too. I knew from that experience that I wanted to be in a profession that helped people. My dad was a surgeon so I thought maybe I could be a physician. I took an organic chemistry class in college and it did not go well; I dropped the class. So medicine was out, but I found psychology. It all just made sense. I knew I wanted to go to grad school and I wanted to specialize in anxiety.
Were there any experiences early on in your career that were particularly profound?
Jerry: I did my post-doctoral training at a place called the Bio Behavioral Institute in New York. They were hard-core behaviorists, pioneers in the field, and I really developed my niche in OCD and anxiety with them. But they were uncompromising. We would have sessions in dumpsters with people who were afraid of germs. It was fascinating to see how people would find the courage to do these things because they had faith that the treatment would work. It was very rewarding. It’s definitely not a 9-to-5 job, thinking about creative ways to get people to face their fears.
Why did you decide specifically to focus on working with young people?
Jerry: In part because I love young people so much. I’ve always bonded with kids. I can pick up a screaming baby and kind of soothe it. People call me the baby whisperer. I’m an adult but I have the sense of humor of a twelve-year-old boy at times, so I can relate to kids. And I always feel if we can get to people when they’re young and give them strategies and skills — like what my parents indirectly taught me about overcoming fear — then we can pave the road to a lifetime of happiness.
When you started applying what you were learning to kids, how was it different and exciting?
Jerry: The thing I learned while working with kids is that you can’t use the psychobabble that you use with adults. You have to break the topics down into a language the kids can understand. And I found that the more I did that, and the more that they were understanding the conceptual models of what we were doing and really making progress, then I would start to use the same metaphors and language with adults. Working with kids made me more effective working with adults because we had to talk about things in real language. In this field, we tend to take simple ideas and put crazy language to them because it makes us feel more important or something. But with kids you can’t do that.
Kids like to call you out.
Jerry: Yes. You can’t mess around with a kid. They don’t necessarily have the same filter that adults would have. I could say something pretty boneheaded right now and you might think, “Maybe I shouldn’t mention it.” But a nine-year-old is going to come out and say “that’s stupid, why did you say that?” (Laughs.) So they keep you on your toes.
[insert page=’donate-cta-story-jerry’ display=’single-multimod.php’]
How did you become the OCD guy?
Jerry: When I was in training, I wrote a book on compulsive hoarding, which got my name out into the OCD community because hoarding was associated with OCD at the time. I met a lot of the leaders in the field and pioneers in the field, and the more I got to know OCD, the more I bonded with OCD. Maybe because of my own phobias and my training, I understood how OCD worked. It’s very synonymous in presentation and style in treatment response to phobias.
When a kid walks into your office, how does the conversation go?
Jerry: I ask about their interests and what they like and if they’re sports fans. It’s a way to bond and get to know them. There’s a school of thought that you shouldn’t disclose a whole lot about your personal life to your patients — that you’re the doctor and they’re the patient and it’s all about them. But that doesn’t always work with kids. They have to understand a little bit about who you are. So I talk a lot about my past, my fear of dogs. I talk a lot about sports and the teams I like. I’m from Minnesota so unfortunately I’m used to losing a lot in sports. And that helps kids kind of feel more comfortable with me. The sessions don’t always feel so clinical, they’re also kind of establishing more of a personal relationship. Normally in sessions my tie is loose, my collar is unbuttoned, my sleeves are rolled up, and I’m not the doctor, I’m Jerry.
How does it feel being involved in changing a kid’s life?
Jerry: Well, I think that’s why we all get in this line of work. I like getting paid for doing what I do but really the reason is knowing that you’re making a difference in someone’s life. And that they come to us in a very acute crisis mode. Their lives are in shambles. They’re not going to school, and if they are, they’re not doing very well. They’re not going out with their friends, they’re caught up in their symptoms, their rituals, their avoidances. So they come to us at a very troubled time. Often times they’ve been to different therapists and doctors and nothing’s really worked. We hear a lot that we are sometimes their last hope. So to be able to connect with someone, to have them believe that I’m going to be able to make a difference in their life, is very powerful. It puts a lot of responsibility onto me, which I welcome and respect. I think they see that and it allows them to commit to the relationship and to the treatment. It feels amazing to see someone who’s really struggling become the person they used to be. And parents saying, “We have him back. He’s back to being our son.” It’s very powerful.
Learn more about our Family Resource Center and our editorial mission.
Was this article helpful?
Related Reading
-
 Complete Guide to OCD
Children with OCD have intrusive thoughts and worries that make them extremely anxious, and they…
Complete Guide to OCD
Children with OCD have intrusive thoughts and worries that make them extremely anxious, and they…
-
 What Is Relationship OCD (R-OCD)?
How this kind of anxiety can make romantic relationships difficult for teens
What Is Relationship OCD (R-OCD)?
How this kind of anxiety can make romantic relationships difficult for teens
-
 When OCD Triggers Suicidal Thoughts
How a form of OCD can be mistaken for being suicidal
When OCD Triggers Suicidal Thoughts
How a form of OCD can be mistaken for being suicidal
-
 Understanding Religious OCD
When the motivation is anxiety, not faith
Understanding Religious OCD
When the motivation is anxiety, not faith
-
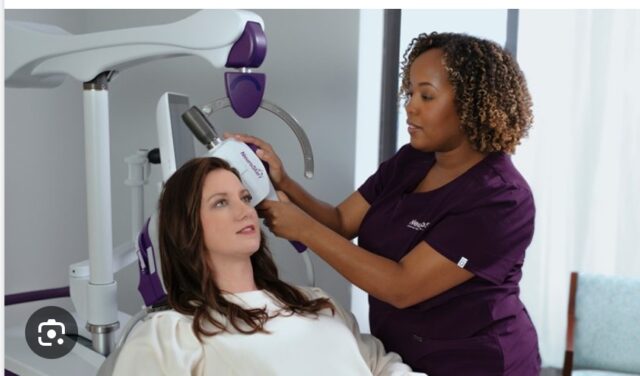 TMS Treatment for Depression
Magnetic brain stimulation can help adolescents with persistent depression
TMS Treatment for Depression
Magnetic brain stimulation can help adolescents with persistent depression
-
 OCD Test for Kids and Teens
Our free Symptom Checker can help you determine if your child might have OCD
OCD Test for Kids and Teens
Our free Symptom Checker can help you determine if your child might have OCD
-
 How Matt’s Loss Made Him Stronger
Overcoming OCD and trauma with treatment and support
How Matt’s Loss Made Him Stronger
Overcoming OCD and trauma with treatment and support
-
 Mental Compulsions and “Pure O” OCD
Almost all kids with OCD experience compulsions, but some kinds are easy to miss
Mental Compulsions and “Pure O” OCD
Almost all kids with OCD experience compulsions, but some kinds are easy to miss








